“Governments have put a lot of money into developing these vaccines. It's a dilemma with legal, economic, political and ethical aspects. The key would be for pharmaceutical companies to allocate part of their profits to more universal and equitable access to vaccines”.
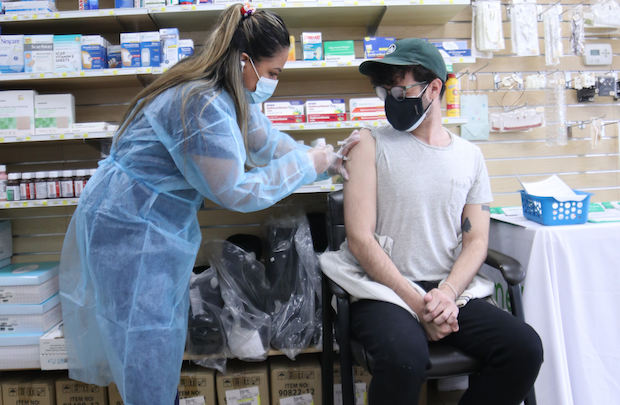
![Photo: [link]Mufid Majnun[/link], Unsplash CC0.](https://cms.evangelicalfocus.com/upload/imagenes/60dc8d844eab8_mufidmajnuncor.png) Photo: [link]Mufid Majnun[/link], Unsplash CC0.
Photo: [link]Mufid Majnun[/link], Unsplash CC0.
Last May, 62 countries supported a revision of the October 2020 proposal by India and South Africa to abolish patents on coronavirus vaccines, and the document reached the World Trade Organization (WTO), opening a new discussion on intellectual property rights for medicines.
The magnitude of the debate expanded after the United States supported a temporary patent waiver for coronavirus vaccines. “These extraordinary times and circumstances call for extraordinary measures. The US supports the waiver of IP protections on COVID-19 vaccines to help end the pandemic”, said US Trade Ambassador Katherine Tai.
The European Union has refused to support Washington D.C.'s proposal to liberalise patents, even though the EU Biotechnology Directive 98/44EC states that “the law must be applied so as to respect the fundamental principles safeguarding the dignity and integrity of the person”, and that “inventions must be excluded from patentability where their commercial exploitation offends against order public or morality”.
This is not the first time that this debate has come to the forefront of public arena. In 2001, the WTO adopted the Doha Declaration, which implied a commitment to make intellectual property more flexible with the aim of ensuring equitable access to pharmaceuticals.
That agreement stated that each member country had the power to determine a national emergency situation, in which the intellectual property rights of medicines could be temporarily affected, and that health crises such as HIV or malaria could be considered in such cases.
“The right of governments to take the necessary measures to eliminate patents and prioritise public health over the economic interests of the pharmaceutical industry was recognised”, recalls Rosa López, a nurse and head of the Bioethics Committee of the Spanish Evangelical Alliance (AEE).
Another milestone in the history of the debate on patents on medicines is the one on Hepatitis B drugs in the 1980s. However, the magnitude of coronavirus and its pandemic nature make it necessary to take into account all the details when analysing the issue.
A controversial aspects to consider is the process of producing a coronavirus vaccine. For example, the Pfizer-BioNTech vaccine requires up to 280 components supplied by 86 suppliers from 19 different countries.
One of the key elements of the vaccine produced by this company and also by Moderna, is the use of ribonucleic acid to achieve the development of an immune response, known as messenger RNA technology, and it is the result of years of joint research and development between the public and private sectors.
Spanish National Biotechnology Centre researcher Daniel Fernandez believes that “even if patents were released tomorrow, starting the whole process from scratch to produce them in other companies in other countries would take a long time. Apart from releasing the patent, you need to get the technology and processes to produce it, set up facilities and do all the checks to make sure the product is safe. It is not clear that the whole process will happen in time to have an effect on current vaccination”.
One example of this is the agreement between AstraZeneca and the Serum Institute of India, for the latter to produce and distribute the majority of the British company's doses.
Or the Bolivian government's agreement with the Canadian company Biolyse Pharma Corporation to supply the South American country with 15 million doses of Johnson & Johnson, which has led the Bolivian government to initiate a licensing procedure before the WTO.
Considering that “current legislation protects intellectual property”, López points out that it is necessary to make an effort at this time of pandemic to “reconcile and prioritise the right to access to health”.
“In order to have a fair access to vaccines, supporting each country in its specific needs, thinking about logistics, transport, storage and conservation, as well as the human resources necessary for large-scale vaccination, the solidarity and collaboration of everyone is needed”, she adds.
Fernández underlines that the current debate on patent liberalisation “can be used as an element of pressure in negotiations with pharmaceutical companies to achieve a fairer price”, but “I find it hard to imagine that there will be a temporary suppression of the intellectual property of coronavirus vaccines", because "it can be complicated to decide which patents to release and which not to release”.
The coronavirus pandemic has generated other conflicts related to the use of patents that have nothing to do with vaccines..
For example, the lawsuit brought by Labrador Diagnostics LLC against BioFire Diagnostics for patent infringement in the diagnostic testing of coronavirus. The lawsuit was eventually dropped and aroused a lot of hostility from the public.
Or the controversy over statements, later denied, by a patent holder against a group of people making parts of ventilators with a 3D printer to be used in Italian hospitals. Although the statement was not true, it did generate a new perspective in the debate on how coronavirus affected the intellectual property of certain products.
However, one of the most complex particularities concerning vaccines is the relationship between the public and private sectors and the investments of both in the drug development process.
According to data collected by The Lancet, and later released by Médecins Sans Frontières, more than $10 billion of public money has been invested in private companies for R&D, clinical trials and the manufacture of six coronavirus vaccines.
The research shows that AstraZeneca and Oxford University have received more than $1.7 billion; Johnson & Johnson more than $1.5 billion; Pfizer-BioNTech more than $500 million; GlaxoSmithKline-Sanofi Pasteur about $2.1 billion; Novavax-Serum Institute about $2 billion; and Moderna-Lonza about $2.48 billion to develop their drugs.
“Governments have put a lot of money into developing these vaccines. It's a dilemma with legal, economic, political and ethical aspects. The key would be for pharmaceutical companies to allocate part of their profits to more universal and equitable access to vaccines”, says López.
The head of the AEE Bioethics Committee explains that “some pharmaceutical companies have given millions of doses to low-income countries and are developing forms of collaboration that allow them to expand vaccine production”.
For Fernández “the reality is that most of the basic research that leads to the development of a drug starts in public research centres”. “But the most advanced phases, the clinical trials, are too expensive, a large economic investment with little chance of success, so that the states in general cannot afford them”.
That investment “is made by industry, which does have the money and infrastructure to do so, and is the one that ends up benefiting from the exclusivity that the patent provides”, he points out.
According to Fernández, releasing vaccine patents “will not affect basic research”, although “it may make companies not want to invest in taking the results of the research to the final development of the drug”. “If they can get out of it and still benefit from it, there is no incentive to take on such an investment with all the risk it entails”.
This, the researcher points out, can affect “the ability to translate that scientific research into concrete products that have an effect on people”.
“With an industry that only sees investing in science as a big risk with no potential benefits, the clinical phase of research can be crippled. States, but also NGOs and foundations, are willing to invest money in improving the health of the population, but companies and investors are not”, he says.
The head of the AEE Bioethics Commission stresses that “if the motivation of the investigation is to respond to people's real needs, there have to be policies and agreements to ensure that it reaches all people, avoiding economic barriers. The needs of the most vulnerable cannot be alien to us”.
“From a more selfish point of view, we live in a global world and what happens in one place affects the rest. The coronavirus has highlighted how no one is safe unless we are all safe”, she insists.
Bioethical reflection has been marginalised in the legal and economic approaches to patents and intellectual property. But in the case of the coronavirus pandemic, this aspect has also been taken into account in formulating a comprehensive reflection on the issue.
“The debate on patent liberalisation is good and makes sense, but a deeper reflection is needed. If we stay there, we are only thinking about the privileges that others have and what they can do to improve the situation and make vaccination fairer and more accessible to all. But we can also reflect on what privileges we have and what we can do”, says Fernández.
For him, “the European Union has been an example of internal solidarity, ensuring that all member states have equal access to vaccines”, but “why have we not been equally supportive of others? Why is it that when we hear about donating vaccines, we refer to a particular brand because we don't like it, and we give what we have left over?”.
“If we want to demand solidarity from industry, we could start by showing solidarity as countries. We could lead by example. It would be a very positive thing if this specific debate makes us look inwards and reflect more generally, as a country, and also each of us, on whether we care enough about others, or whether we are living a life for ourselves”, underlines Fernandez.
Rosa López points out that “we all belong to the human race and that is reason enough for us to care about others. The greatest sunk investment ever made was made by God sending Christ to stand in our place”.
That is why “raising our voices for those who have no voice and no resources is not unusual, it is the natural consequence of having understood the message of the gospel and being disciples of Jesus”.
“Jesus always took the side of the weakest, including you and me”. “From a Christian worldview, love is the key, treating others as Jesus would and as if they were Jesus. I think this goes a step further than solidarity. Sharing with those who don't have, in this case, vaccines, patents, knowledge and resources”, says Lopez.
And adds that “a plan needs to be made to help achieve the goal and to put the resources to good use. The giver is the first beneficiary in the gospel”.
According to the 'Our World in Data' platform, as of 28 June 2021, the European Union has vaccinated 49.87% of its population, while on Africa the percentage drops to 2.62%. In North America, 42.16% of the population has already received their vacine, while in South America only 28.78%.

Las opiniones vertidas por nuestros colaboradores se realizan a nivel personal, pudiendo coincidir o no con la postura de la dirección de Protestante Digital.
Si quieres comentar o